2022 Study: Adipose Augmentation Accelerates Rotator Cuff Recovery After Surgery
Date: 24 February 2026
Admin: Medical Affairs
The Challenge of Rotator Cuff Recovery After Surgery
For active individuals, a rotator cuff tear often feels like a “lifestyle sentence.” The diagnosis brings with it the looming specter of surgery, followed by months of immobilization, physical therapy, and lost seasons of activity.Your ambition isn’t just to endure the recovery; you’re looking for a way to reclaim the quality of movement and freedom that define your day-to-day life.
The frustration lies in the timeline. Even if surgery is successful structurally, the biological healing process is slow. You are often told to “hurry up and wait” while the body attempts to bridge the gap between a surgically repaired tendon and the bone.
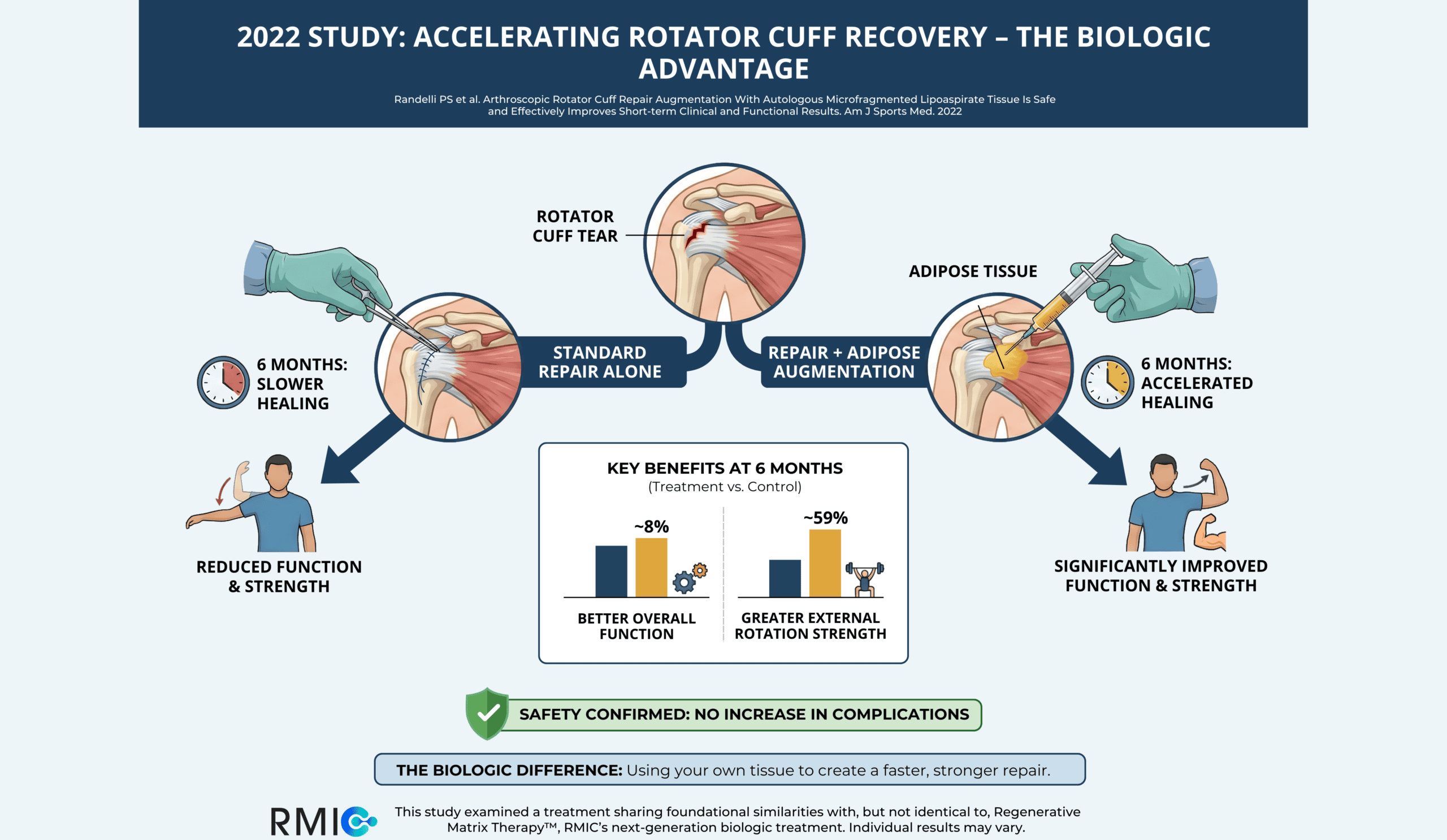
A 2022 randomized controlled trial published in The American Journal of Sports Medicine suggests that your body’s own adipose (fat) tissue may allow you to hit the accelerator on recovery. This study looked at whether adding a patient’s own processed fat tissue at the end of rotator cuff surgery could improve healing. The main result was better function at 6 and 24 months.
The Biology Behind Slow Healing
Rotator cuff tendons, particularly the supraspinatus, suffer from a critical limitation: poor blood supply. This “hypovascular zone” makes healing difficult even when surgery restores the anatomy.
Traditional surgery fixes the structure. A surgeon can stitch the tendon back to the bone with precision, but stitches are only anchors. They hold tissue in place while the body tries to fuse tendon to bone. If the biology is sluggish, the healing process is slow and vulnerable.
Adipose tissue is a biologically active tissue rich in cells such as pericytes and mesenchymal stem cells (MSCs), along with extracellular matrix and other components. When processed, purified and applied to the repair site, adipose tissue may influence the conditions that promote tissue recovery, potentially improving the overall healing process for the tendon.
This study targets an important treatment gap by asking whether a patient’s own adipose tissue can meaningfully improve recovery after surgical repair.
Learn More About Regenerative Matrix Therapy™
Study Overview: A Closer Look at the Trial
- Study Design: Prospective randomized controlled trial of arthroscopic rotator cuff repair with vs without adipose augmentation.
- Population: MRI-confirmed degenerative posterosuperior rotator cuff tears; average age ~59 years; BMI ~25.8; ~59% female.
- Sample Size: 177 screened, 52 randomized, 46 treated, and 44 patients completed 24-month follow-up (22 per group).
- Intervention: All patients had single-row arthroscopic rotator cuff repair. The treatment group additionally received intraoperative injection of autologous microfragmented adipose tissue.
- Follow-Up: Clinical assessments at 3, 6, 12, 18, and 24 months; MRI at 18 months to assess tendon integrity and tears.
- Primary Endpoint: Shoulder function at 6 months measured by the Constant–Murley Score.
Key Findings: Faster, Stronger Early Recovery
The most significant outcome from this study is the remarkable early recovery observed in patients who received adipose augmentation. Although both groups showed improvement over time, those in the treatment group not only recovered more quickly but also achieved greater functional gains within the crucial first six months following intervention. This accelerated progress is particularly important for patients aiming to return to daily activities, sports, and other demanding tasks.
- Improved Shoulder Function at 6 Months:
The Constant–Murley Score, which comprehensively assesses pain, daily activities, range of motion, and strength, demonstrated substantial improvement in both groups. However, the treatment group exhibited a notably greater enhancement, improving by ~68% from baseline to 6 months (49.3 → 82.8; p < 0.0001), compared to a 34% improvement in the control group (57.3 → 76.7; p < 0.0001). At the end-point, shoulder function was about 8% higher in the treatment group (82.8 points) than in the control group (76.7 points; p = 0.005). These statistics highlight the superior recovery trajectory associated with adipose augmentation.
Why It Matters: Achieving higher shoulder function scores at 6 months translates to improved real-world performance during the period when patients are eager to resume normal routines and physical activities.
- Strength Gains Where It Counts
Objective strength testing revealed marked differences between groups. External rotation strength, crucial for sports such as golf and tennis as well as overhead tasks, was significantly greater in the treatment group. Specifically, external rotation strength was ~59% higher in the treatment group compared to controls (6.06 kg vs 3.80 kg; p = 0.0077). Early restoration of this strength is often the bottleneck for return to sport and other activities requiring robust shoulder function.
- Daily Activities and Confidence
The Constant–Murley daily activity subscale, which encompasses tasks like dressing, reaching, and sleeping, showed a pronounced early improvement in the treatment group. Daily activity scores improved by ~126% from baseline to 6 months (8.65 → 19.57), with a statistically significant difference favouring the treatment group at 6 months (p = 0.0037). These gains reflect enhanced confidence and independence in everyday life.
- Pain Reduction and Long-Term Outcomes
Both groups experienced substantial pain reduction by 6 months, but the treatment group saw a greater decrease. Pain scores dropped by about 90% (52.0 → 5.1) in the treatment group and approximately 73% in the control group. By 24 months, shoulder function scores were similar between groups (Constant–Murley 86.3 vs 84.5; p = 0.563), indicating durable outcomes. MRI-confirmed retear rates were lower in the treatment group (9.1% vs 17.4% in controls), though this difference was not statistically significant due to limited sample size.
- Excellent Safety Profile
Importantly, no serious adverse events were reported, and no complications were definitively attributed to the fat harvesting procedure. This underscores the favourable safety profile of the intervention.
Start Your Virtual Consultation
What This Means for You: Shifting the Recovery Curve
If you are facing rotator cuff surgery and value time, function, and confidence, this study highlights an important concept: biology matters as much as mechanics.
Adding microfragmented adipose tissue did not change the surgery itself. It changed the timeline in which healing occurred. Patients who received augmentation reached higher functional levels sooner, particularly in daily activities and strength, during the critical early months of recovery.
At the same time, it is important to be candid. By two years, outcomes between groups looked similar, and retear rates were directionally superior but not statistically different due to the small sample size. This approach may help some patients recover faster early on, but conclusions about long-term endpoints will require further research.
This research examined microfragmented adipose tissue augmentation during rotator cuff repair, a treatment that shares foundational similarities with Regenerative Matrix Therapy™, RMIC’s next-generation biologic treatment. Our treatment protocol was reviewed by Health Canada with no objection and is delivered in a physician-led setting focused on safety and outcomes.
Start Your Virtual Consultation
Research Highlights (for clinicians)
Study Design: Prospective randomized controlled trial; single-row arthroscopic rotator cuff repair with or without intraoperative autologous microfragmented lipoaspirate (Lipogems).
Population: 44 patients with degenerative posterosuperior rotator cuff tears; 22 per group completed 24 months.
Primary Outcome: Constant–Murley Score at 6 months. MRI at 18 months (n = 45).
Effect Size: Approximately 8% higher Constant–Murley Score at 6 months with augmentation (82.8 vs 76.7; p = 0.005). Daily activity subscale favored treatment at 6 months (p = 0.0037; Bonferroni-adjusted p = 0.0296). No between-group difference at 24 months.
Safety: No serious adverse events; no harvest-related adverse events attributed with certainty.
Limitations: Small sample size, unblinded patients, multiple comparisons, surgical context limits generalizability.
Citation: Randelli PS, Cucchi D, Fossati C, et al. Arthroscopic Rotator Cuff Repair Augmentation With Autologous Microfragmented Lipoaspirate Tissue Is Safe and Effectively Improves Short-term Clinical and Functional Results. Am J Sports Med. 2022;50(5):1344–1357. doi:10.1177/03635465221083324.
Learn More About Regenerative Matrix Therapy™See More Conditions We Treat
Disclaimer
Regenerative Matrix Therapy™ shares foundational similarities with, but is not identical to, the treatment studied. Individual results vary based on disease severity, anatomy, and adherence to post-care protocols. Educational content only; not a substitute for professional medical advice.
Why Choose Regenerative Matrix Therapy™ with RMIC?
At RMIC, Regenerative Matrix Therapy™ is delivered via a standard, physician-led protocol built on years of orthobiologic experience and direct dialogue with Health Canada. Our patent-pending, adipose-based approach was reviewed by Health Canada with no objection, and is built around safety, efficacy, and realistic expectations.
If you’re exploring advanced, non-surgical options to help manage rotator cuff tears or shoulder degeneration and preserve your lifestyle, find out whether Regenerative Matrix Therapy™ is a good fit for you.